The Impact of Being Homeless on the Unsuccessful Outcome of Treatment of Pulmonary TB in São Paulo State, Brazil
BACKGROUND:
Tuberculosis
(TB) is a major public health problem requiring complex treatment, the success
of which depends on biological, social, and institutional factors. São Paulo
State (SPS), in Brazil, has a high TB burden. Because of high socioeconomic
heterogeneity and chaotic urbanisation, homelessness might play an important
role in the TB burden in SPS. Our aim was to determine the association between
homelessness and outcome of treatment of pulmonary TB (PTB) in SPS.
METHODS:
A
historical cohort from the routine SPS TB database for 2009-2013 was analysed.
The study population was newly diagnosed adult patients with PTB. Homelessness
was ascertained at notification or when treatment started. Our outcome was
unsuccessful outcome of treatment. We used logistic regression to adjust for
potential confounders and multiple imputation for missing data.
RESULTS:
We
analysed 61,817 patients; 1726 (2.8 %, 95%CI 2.7-2.9 %) were homeless. Homeless patients were concentrated in bigger cities,
were more frequently middle-aged males, had black/brown skin colour, and had
received less education (P < 0.001, for all). Alcohol and drug use was three
times more frequent in homeless patients
(43.2 % vs 14.4 %, 30.2 % vs. 9.4 %, P < 0.001, respectively). HIV testing
was less common among the homeless, of whom 17.3 % were HIV positive compared
with 8.5 % among the not homeless population
(P < 0.001). Microbiologic confirmation was more frequent among the homeless (91.6 % vs. 84.8 %, P < 0.001).
Unsuccessful outcome of treatment was 57.3 % among thehomeless and 17.5 % among the not homeless (OR = 6.32, 95%CI 5.73-6.97, P < 0.001),
mainly due to loss to follow-up (39 %) and death (10.5 %). After
full-adjustment for potential confounders, homelessness remained strongly
associated with lower treatment success (aOR = 4.96, 95 % CI 4.27-5.76, P < 0.001).
HIV status interacted with homelessness: among HIV-infected patients, the aOR
was 2.45 (95%CI 1.90-3.16, Pinteraction < 0.001). The population
attributable fraction for the joint effect of homelessness, alcohol and drug
use was almost 20 %.
CONCLUSIONS:
Confirming
our hypothesis, homelessness led to a marked reduction in the successful
treatment of newly diagnosed pulmonary tuberculosis. Homelessness and
associated conditions were important contributors to lack of treatment success
in pulmonary tuberculosis in São Paulo. A multifaceted intervention must be
implemented to target this vulnerable population.
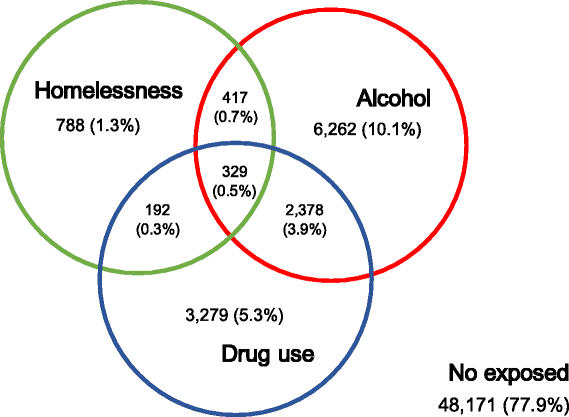
Below: Intersection between homelessness, alcohol use and drug use
- 1Pulmonary Division, Heart Institute (InCor), Medical School, University of São Paulo, Av. Dr. Arnaldo, 455, 2° andar, sala 2144, Post-code 01246903, São Paulo, Brazil. otavioranzani@yahoo.com.br.
- 2London School of Hygiene & Tropical Medicine (LSHTM), Keppel Street, Room G9a, Post-code WC1E 7HT, London, UK. otavioranzani@yahoo.com.br.
- 3Pulmonary Division, Heart Institute (InCor), Medical School, University of São Paulo, Av. Dr. Arnaldo, 455, 2° andar, sala 2144, Post-code 01246903, São Paulo, Brazil.
- 4Department of Epidemiology, Faculty of Public Health, University of Sao Paulo, Av. Dr. Arnaldo, 715, Post-code 01246904, São Paulo, Brazil.
- 5London School of Hygiene & Tropical Medicine (LSHTM), Keppel Street, Room G9a, Post-code WC1E 7HT, London, UK.
- BMC Med. 2016 Mar 23;14(1):41. doi: 10.1186/s12916-016-0584-8.
No comments:
Post a Comment